Holiday Relapse Triggers & Emotional Stress | Freeman Recovery Center
It’s the most wonderful time of the year — or the most challenging for the 48.5 million Americans who battle a substance use disorder. During this time, there are countless parties for celebration, family and friends to commiserate with, and festive alcoholic beverages and food around. However, the very reasons why the holiday season can be so joyous for some can be the very reasons why relapse feels inevitable for others. Instead of appearing like a Scrooge or a Grinch, many suffer in silence, or in some cases, relapse entirely.
Because holiday celebrations are so ingrained in American culture, it can be challenging to pinpoint what exactly exacerbates substance use behaviors around this time of year. However, we wanted to figure out why. To do so, we surveyed over 1,000 Americans about how they genuinely feel about the holidays and whether the season impacted their substance use habits. The results revealed that for many, substances like alcohol weren’t just part of holiday parties, but a way to endure the season. Read on to uncover what really drives holiday relapse risk, from grief and loneliness to social pressure and beyond.
Key Takeaways
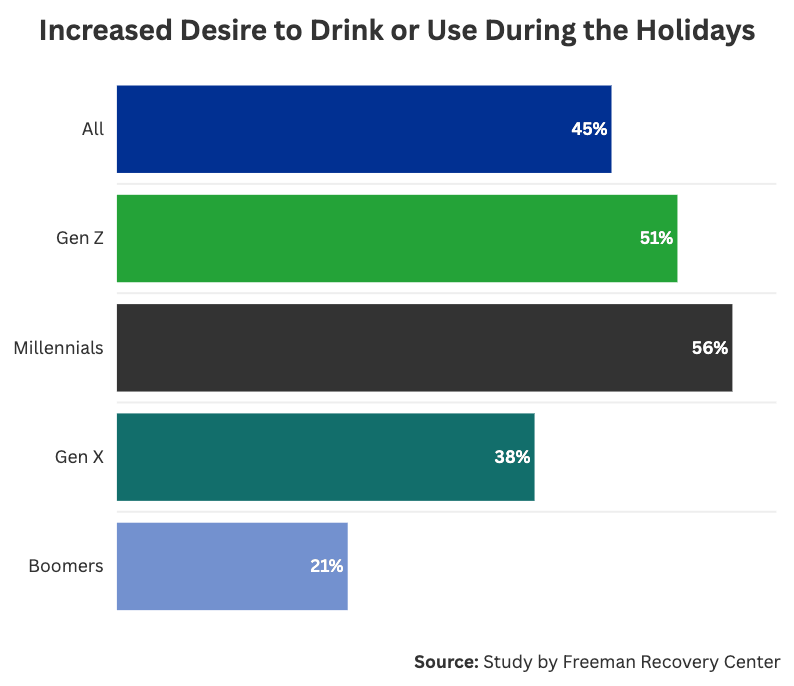
- Up to 45% of Americans say their urge to drink or use increases during the holidays, rising to 51% for Gen Z, 56% for millennials, and 73% among those with a substance use history.
- Half of Americans pre-game to take the edge off before holiday family gatherings, with 51% drinking beforehand, and about one in three using cannabis, rising to 43% among Gen Z and millennials.
- Nearly three in four Americans (73%) say the holidays trigger emotions tied to a past loss, and 57% say they experience emotional hangovers after holiday events — most common among millennials (66%) and Gen Z (60%).
- 74% feel lonely at least some of the time during the holidays. Nearly half of Gen Z (42%) turn to social media or doomscrolling to cope with holiday loneliness — more than any other generation.
- Half of Americans use substances to cope with holiday financial stress, including 40% who turn to alcohol and 33% to cannabis, while two in five adults hide holiday purchases or debt, most often from a partner (28%).
- About 1 in 4 Americans feel pressured to drink or use substances at holiday gatherings, rising to 1 in 3 among Gen Z and millennials.
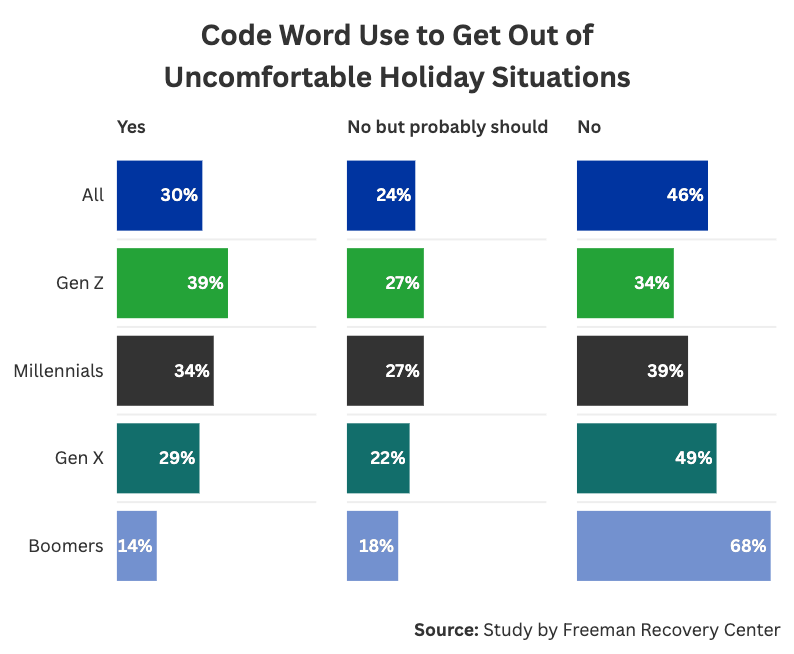
- One in four Americans (23%) skip holiday gatherings to avoid heavy substance use. Of those who attend, 30% have a code word or signal to de-escalate or exit if things get uncomfortable.
Holiday Substance Cravings and Pre-Gaming
For many Americans, the holidays spark seasonal cravings for eggnog, deviled eggs, and cranberry sauce. For others, the stressors that come with the holidays incite a craving for alcohol, cannabis, prescription drugs, and other substances. These emotional stressors are present long before anyone takes a drink. At family holiday gatherings, 36% of Americans describe themselves as “stressed but manageable,” 15% feel “overwhelmed or emotionally triggered,” and 9% feel “disconnected or numb.”
For respondents who reported a substance use history, the emotional load is even heavier: just 19% feel calm and connected, while 38% feel stressed, 22% feel triggered, and 15% feel numb.
Even without an alcohol use disorder diagnosis, many people often normalize alcohol misuse around the holidays and even pressure others to do so as well. Our survey revealed that nearly half of Americans (47%) feel pressured at least sometimes to drink or use substances at holiday events; this climbs to around three in four among those with a substance use history.
However, if we remove social pressures, the holidays can directly increase our cravings for vices. We found that 45% of Americans say their desire or temptation to drink or use increases during the November–December holidays; 17% say it increases significantly, and 28% say it increases slightly. For those with a history of substance use disorders in the survey, 72% say their desire to drink or use increases during the holidays.
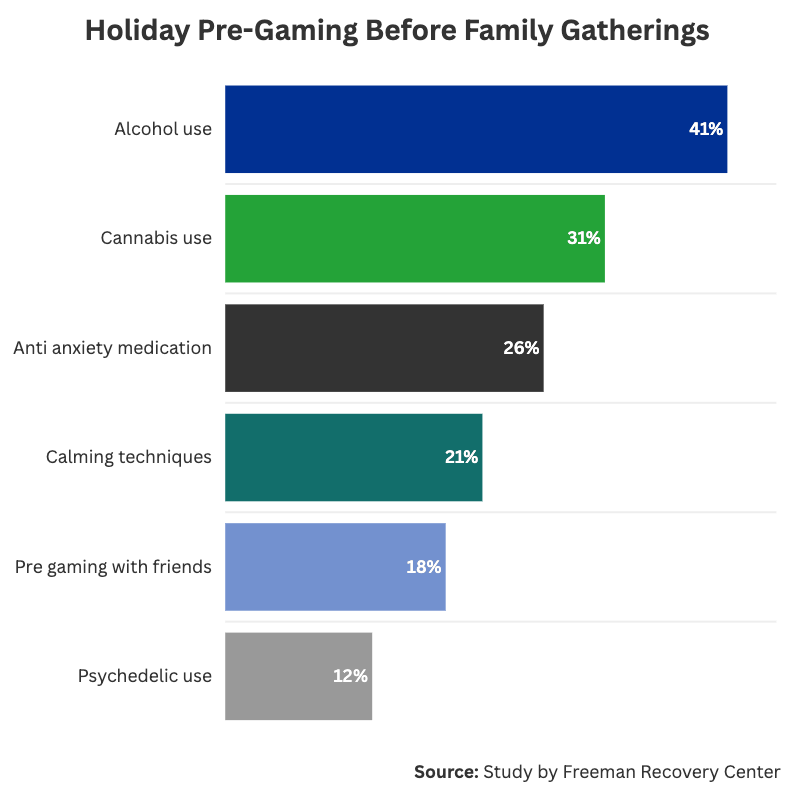
During the holidays, many survey respondents talked about “pre-gaming” before holiday celebrations, which involves consuming substances before celebrations begin. It is also a symptom of substance use disorder. Before holiday family gatherings, 41% of Americans say they have pre-gamed to prepare emotionally by drinking alcohol, 31% by using cannabis, and 12% by using psychedelics or other mood-altering substances. This activity was also far more common for those with a substance use history, with 66% drinking, 48% using cannabis, and 24% using psychedelics before holiday family events.
Grief, Loneliness, and Emotional Hangovers During the Holidays
For many people, the holidays are a time when they can reflect on holidays of years past and the memories made with loved ones. However, for many, the holidays can bring feelings of grief or loneliness if you’ve lost someone or if you’re alone.
On the flipside, if you’ve spent weeks surrounded by family, returning to your routine can present an “emotional hangover” that can derail your life. We found all of these emotional responses in our survey, especially among those with substance use disorders, indicating that grief, stress, and loneliness can all be factors behind relapses.
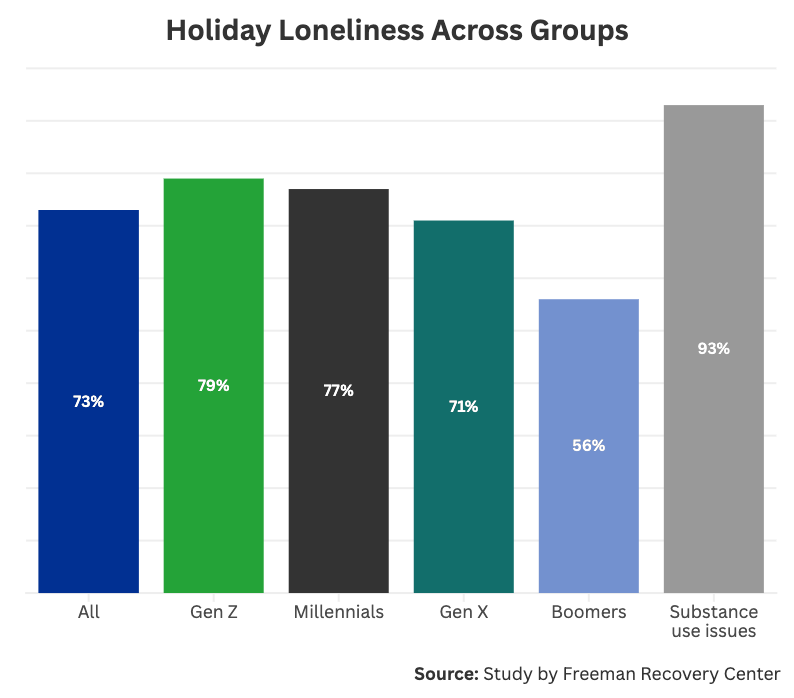
For those who surround themselves with loved ones but may be struggling with mental health disorders, such as depression, loneliness can be a common feeling during the holidays. In our survey, we found that 73% of Americans feel emotionally isolated or lonely at least sometimes during the holiday season. Among those with substance use disorders, 93% reported feeling lonely at least sometimes. Each generation also experienced holiday loneliness, with about 79% of Gen Z, 77% of millennials, 71% of Gen X, and 56% of baby boomers feeling lonely at least sometimes.
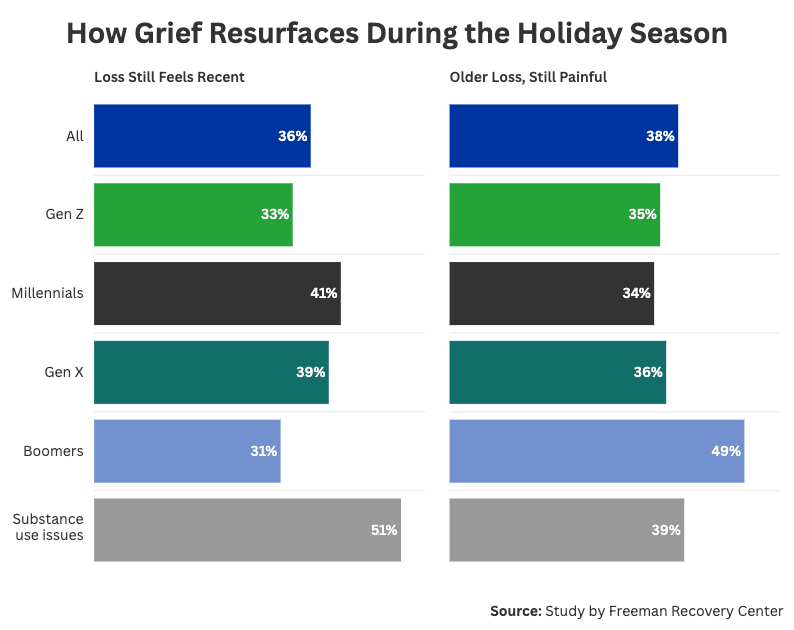
Loss was ubiquitous in our survey. Up to 74% of Americans say they have lost a loved one whose absence still emotionally impacts them during the holidays; 36% say the loss still feels recent, and 38% say it’s older but still resurfaces. Among people with a substance use history, 90% carry grief into the holidays, with 51% saying the loss still feels recent and 39% saying it is older but still painful.
While every generation felt some level of grief during the holidays, the way it felt differed for each generation. For example, 41% of millennials said their loss still felt recent, while 49% of baby boomers said the loss occurred a while ago, but the holidays still brought back the grief. For baby boomers, it didn’t matter how long they’ve been experiencing grief; the holidays have the power to bring back feelings they long felt were dormant.
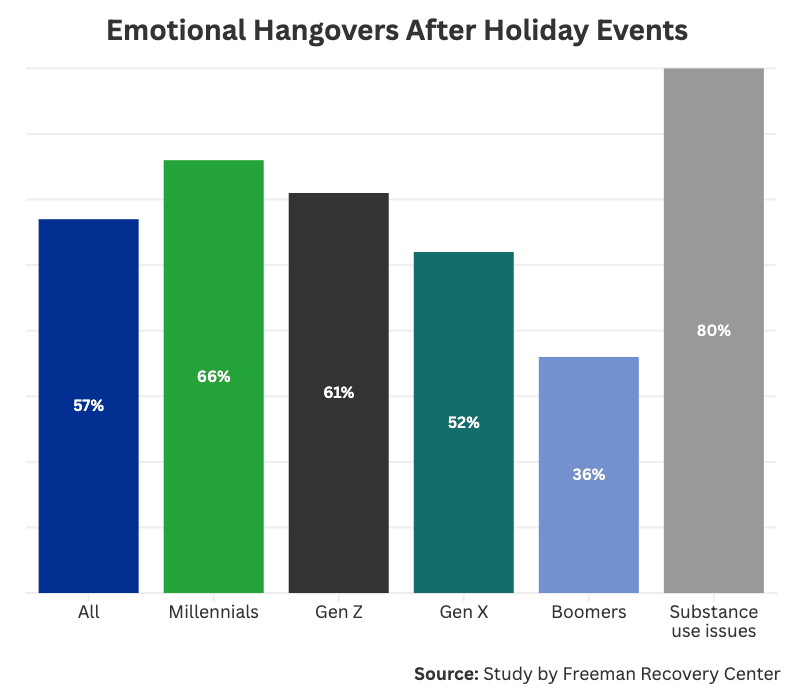
After the last Christmas song plays and the holiday decorations are packed up, the emotional hangover starts to set in. Up to 57% respondents reported feeling emotionally hungover from the holidays. This feeling was more common among younger generations, with 66% of millennials and 61% of Gen Z reporting the feeling.
However, those with substance use disorders reported emotional hangovers the most of any demographic, with 80% reporting the feeling often or sometimes. Since one of the biggest battles with addiction is facing daily life without a quick fix of serotonin, it’s no wonder that people with a history of substance use struggle with the adverse feelings that follow the manic energy surrounding the holidays.
Hidden Holiday Money Stress and Secret Spending
According to a 2024 Gallup survey, the average American spent over $1,000 on holiday gifts.
When faced with this kind of financial stress, many people will turn to substance use to cope and even hide purchases from their family and loved ones.
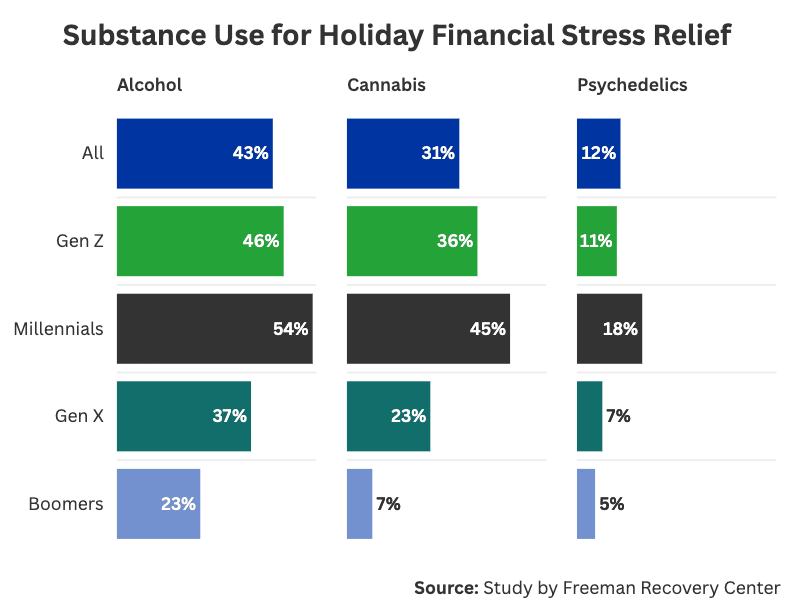
Nearly half (43%) of Americans say they have used alcohol to cope with holiday-related financial stress, 31% have used cannabis, and 12% have used psychedelics or other mood-altering substances. Among those with a substance use history, 68% have used alcohol, 50% cannabis, and 26% psychedelics to manage holiday money stress.
Despite financial stress being a common experience during the holidays, not every generation turned to substances. For example, 42% of Gen X and 68% of baby boomers said they had not used substances to cope with holiday financial pressure. On the other hand, millennials reported the most self-medication when faced with financial stress, with 54% using alcohol and 45% using cannabis.
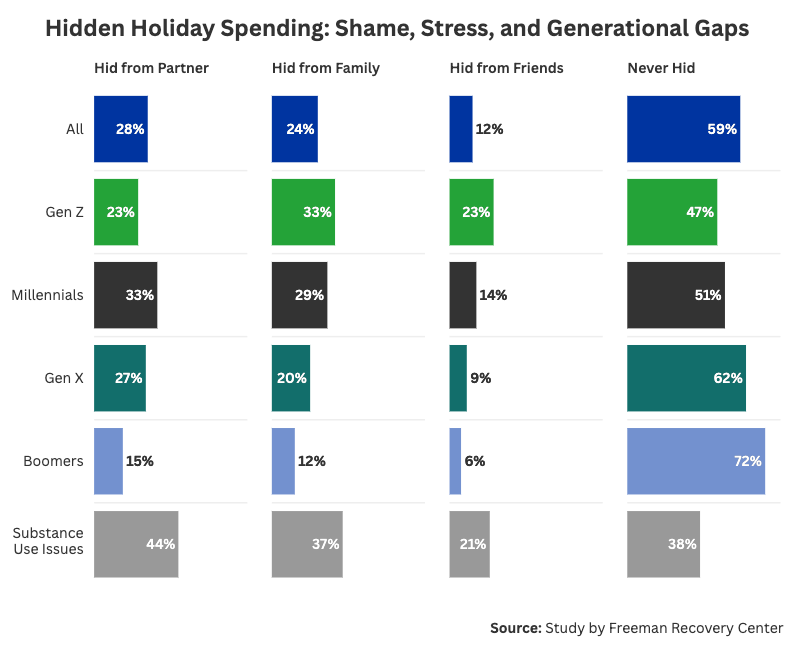
Shame and guilt are common feelings. When faced with these notions, many may try to hide their cause, even from those they love the most. During the holidays, financial shame is even more common, causing Americans to hide their spending. In our survey, 41% of Americans admitted to hiding a holiday-related purchase, expense, or debt from someone close to them, with 28% hiding from a partner, 24% from family, and 12% from friends.
Hiding was even more common among those with a substance use history. This may reflect deeper patterns of financial stress, shame, or the desire to avoid conflict during a high-pressure season. Around 44% have hidden spending from a partner, 37% from family, and 21% from friends; only 38% say they have never hidden holiday money issues from anyone close.
There was also a generational gap in hiding financial spending. Generation Z and millennials were more likely to hide their spending, while an overwhelming 72% of baby boomers reported never hiding financial spending from anyone during the holidays. This fact, in combination with baby boomers’ report on not turning to substance use when faced with financial stress, may indicate that this generation turns to different coping mechanisms when faced with budgetary concerns.
Boundaries, Exit Plans, and Grounding Rituals
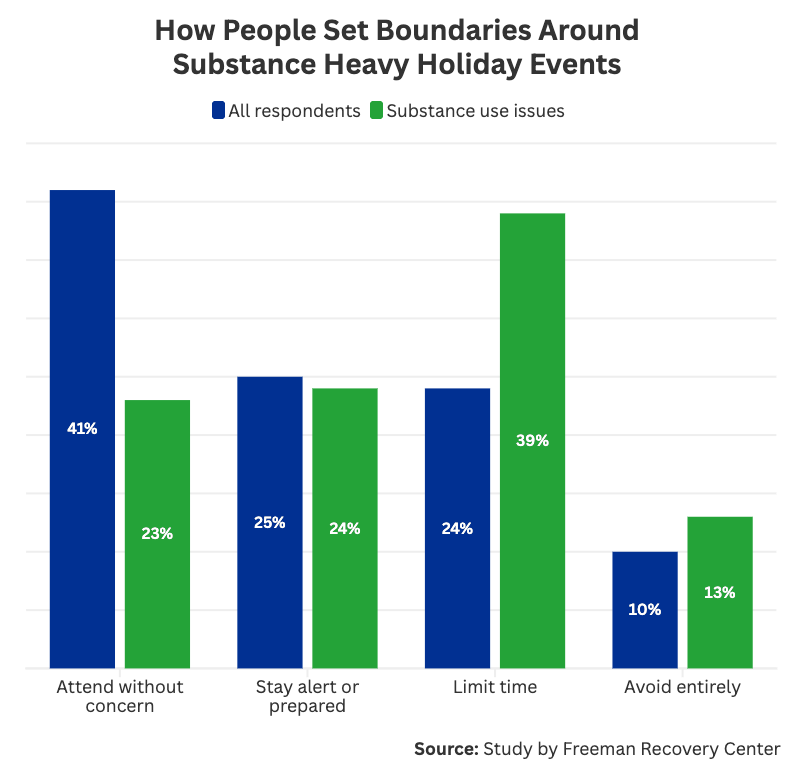
Many Americans simply set more boundaries during the holidays. Avoiding events with alcohol or substances, limiting their time at gatherings, and using secret signals are all common ways to set boundaries among our respondents. Over half (53%) avoided or limited substance-heavy events. Nearly one in four respondents (23%) refrained from any holiday activity in the general public, regardless of whether or not substances would be around. To them, avoiding the holidays altogether was an easier way to maintain sobriety.
However, this response differed across each generation and even among genders. For example, 42% of men were more likely to avoid or limit holiday events where alcohol or substances would be present. In contrast, only 28% of women reported doing the same. Likewise, Gen Z, millennials, and Gen X were more likely to avoid or limit events (36-38%) than baby boomers (24%).
For those who still went to holiday events, using a code word with a loved one was a common way to de-escalate a stressful situation at said holiday event. About 30% of Americans did so; 12% use one regularly, and 18% have used one once or twice. This method was even more common among those with a substance use history, with 46% saying they use a secret signal at least once and only 25% saying they do not.
Survey respondents also had a wide variety of ways to stay grounded. The best way to achieve this differed from person to person, but 35% of respondents said they simply stayed connected with others. Likewise, 27% reported relying on a specific daily routine, 25% avoided known triggers, 12% used mindfulness or spiritual practices, and 3% used professional support to stay emotionally grounded.
More often than not, people with a substance use history would list avoiding known triggers as their top grounding tool, at 33%, compared with 25% overall. To them, steering clear of inflammatory situations was simply the best and most reliable tool for staying stable and sober.
Holiday Coping: Support Systems vs Self-Medication
When it comes to coping, many may think of different strategies in a black-and-white divide. Healthy coping mechanisms, such as reaching out to friends, going to therapy, and practicing mindfulness, sit on one side of the line. Meanwhile, alcohol, cannabis, shopping, and screens lie on the other side. You either use healthy coping mechanisms or you don’t.
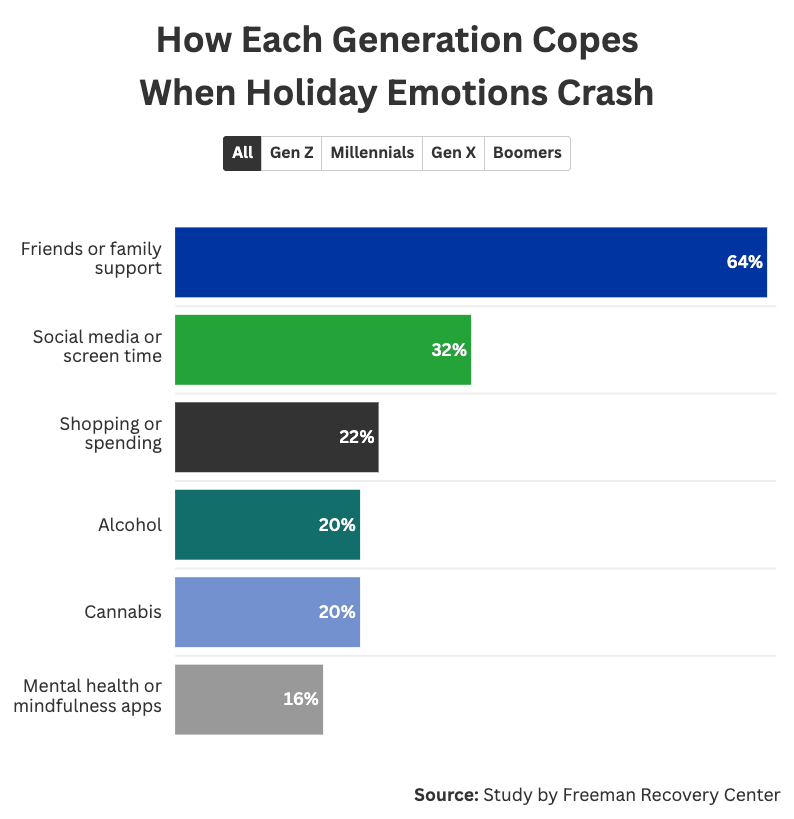
However, around the holiday season, coping can turn a little gray for those who are trying to get through. Even though 64% of Americans turn to friends or family when they feel low, 20% also reach for quick relief through alcohol or cannabis, and 32% disappear into social media or screens.
For people with a substance use history, this gray zone becomes even more pronounced. Many still rely on connection — 62% lean on loved ones — and 23% turn to therapy or recovery meetings for support. At the same time, 29% report using alcohol, 31% report cannabis, and 9% turn to psychedelics when they’re struggling during the holidays.
Younger adults experience a similar tension between grounding habits and escapist ones. Gen Z shows the strongest pull toward emotional connection, with 72% turning to friends or family. Millennials follow close behind at 63%. Yet, both generations still reported screen time as another tool to cope, with 42% of Gen Z and 35% of millennials relying on it. To these younger generations, social connection — whether in person or online — can be the ultimate way to escape the stress of the holidays.
The Holiday Season: A Perfect Storm for Relapse Risk
Taken together, the findings suggest that many individuals experience intensified emotions during the holidays, with particularly pronounced effects among those with a history of substance use. For many, grief, loneliness, financial strain, and social pressure create an emotional load that’s challenging to manage without support. Younger adults felt this most intensely, reporting higher cravings, stronger social pressure, and more emotional overwhelm at holiday gatherings. And while the season brings opportunities to connect and celebrate, it also creates more moments where untreated stress, emotional triggers, and normalized substance use collide.
These patterns reveal the need for proactive, not reactive, holiday mental health planning. Checking in with a friend, attending an additional recovery meeting, or scheduling decompression time may seem minor. However, they are profound ways to protect yourself and establish a support plan that reduces the risk of a relapse. Families and communities can help by reducing pressure to drink, offering alcohol-free options, and normalizing conversations about emotional strain instead of glossing over it. With more awareness and intentional support, the holidays don’t have to be a season people “survive”—they can become a time where joy, connection, and stability are still possible, even for those navigating recovery.
Methodology
We surveyed 1,000 U.S. adults to understand holiday stress, emotional triggers, coping behaviors, and substance use patterns. The sample was stratified and segmented by age, gender, and whether respondents had experienced issues related to substance use. Percentages may not total 100 percent due to rounding.
About Freeman Recovery Center
Freeman Recovery Center provides comprehensive treatment and support for individuals navigating substance use challenges and co-occurring mental health needs. Our programs focus on personalized care, long-term recovery, and strengthening emotional well-being, areas especially relevant during high-stress seasons like the holidays. With a commitment to compassionate, evidence-informed treatment, Freeman Recovery Center helps individuals and families build stability through every stage of recovery.
Fair Use Statement
If you wish to use the information in this article, you may do so for non-commercial purposes only, and attribute with a link back to Freeman Recovery Center.