The Rural Opioid Crisis: Addressing Stigma, Privacy, and Recovery in Small Communities

Image Source: Pexels
The rural opioid crisis is driven by social, cultural, and logistical barriers that differ from those in urban areas.
- Stigma: Fear of judgment or gossip in tight-knit communities can delay or prevent people from seeking treatment.
- Lack of privacy: Concerns about being recognized at clinics or support services discourage ongoing care.
- Cultural norms: Emphasis on self-reliance and distrust of outside institutions can reduce treatment engagement.
- Access gaps: Provider shortages, long travel distances, and limited transportation restrict care options.
Effective solutions must address stigma, privacy concerns, and limited access to care within small, close-knit communities.
- Community-centered strategies: Education and leadership from trusted local voices help reduce stigma and normalize recovery.
- Privacy-preserving care: Telehealth and regional or out-of-community treatment options improve access while protecting anonymity.
- Long-term recovery support: Employment, economic stability, and strong local networks support sustained recovery.
Addressing the rural opioid crisis requires tailored, community-informed approaches that balance access, privacy, and trust.
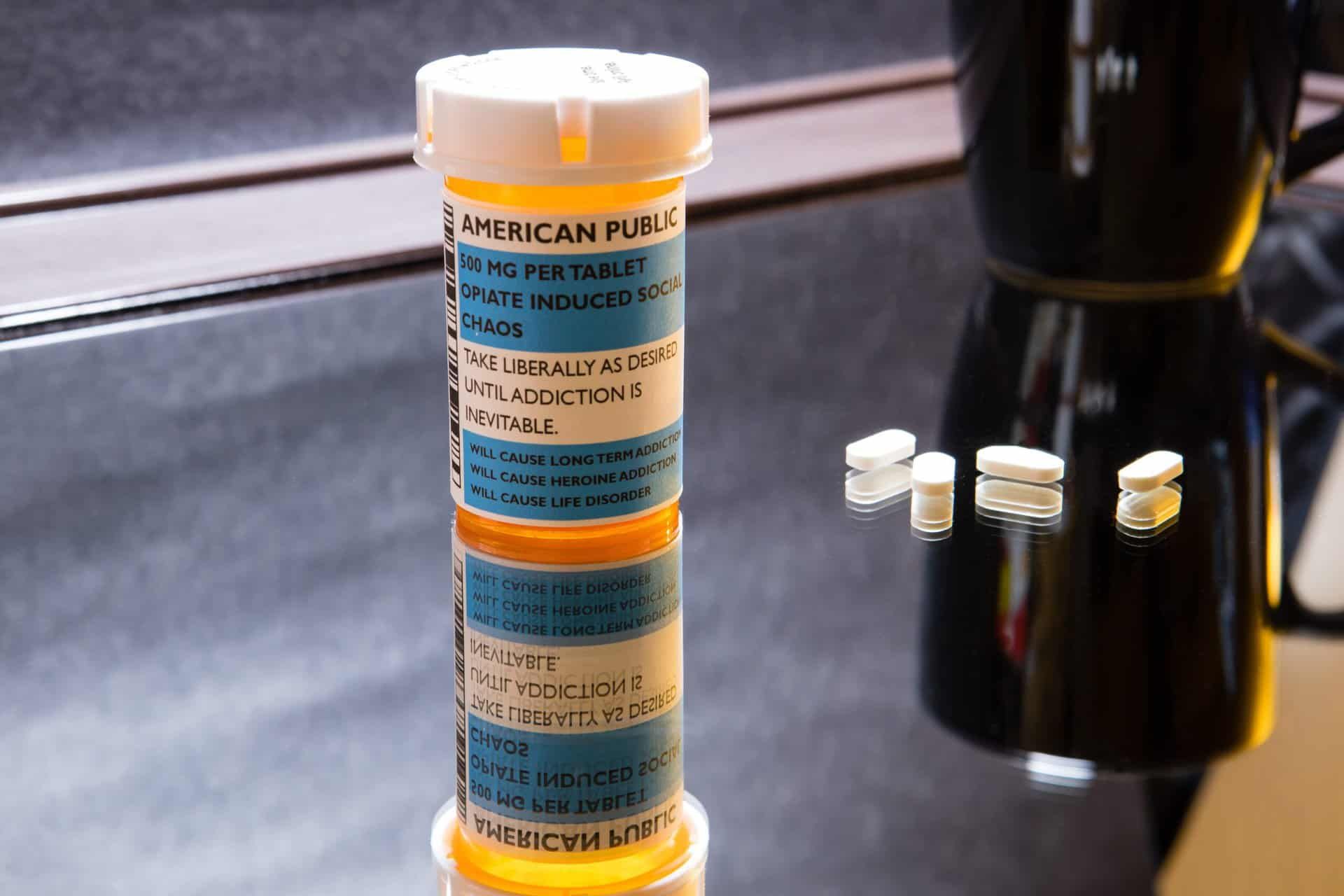
Though it has ravaged the U.S. as a whole, the opioid crisis has had a profound and pronounced impact in rural areas. Research on the opioid crisis compiled by the University of New Hampshire indicates that opioid-related deaths have increased at a much faster rate in rural areas than in urban ones during the opioid prescription peak. Despite seeing a lower rate of opioid deaths overall, prescription opioids are primarily responsible for a higher number of overdose deaths in rural communities compared to urban areas.
It’s difficult to pinpoint precisely why these impacts are more likely to affect rural communities. However, issues like stigma, privacy, and access to care contribute in unique ways compared to urban localities. Properly addressing the opioid crisis in small communities requires a deep understanding of the social and logistical barriers people face when seeking treatment. By learning more about these factors, it’s possible to craft strategies to effectively support rural residents when seeking treatment for opioid use disorder.
Factors That Inhibit Opioid Recovery in Rural Areas
Many factors make it difficult for people to seek treatment for opioid use. However, rural communities face unique barriers that people in urban areas do not face by virtue of their locations. These barriers are often social and cultural as much as they are logistical, and they’re all interconnected.
Some of the most significant factors inhibiting opioid recovery in rural areas include:
Stigma
Stigma is a pervasive issue when it comes to substance use recovery, and it’s especially prevalent in rural areas. Living in a small, tight-knit community can be a double-edged sword. People know their neighbors, but the lack of anonymity can also intensify stigma related to substance use due to overall negative attitudes and beliefs about addiction.
Stigma can cause people to avoid opening up to loved ones or trusted friends for support. Perhaps they’ve heard community members discuss others’ struggles with addiction and fear they’ll be a similar point of gossip; they may have heard their neighbors’ beliefs about addiction itself, with some considering it a moral failing rather than a complex medical condition. Depending on the community, many people may regard substance use as “normal” and feel it isn’t an issue requiring treatment, disparaging those who disagree.
This kind of environment can make the already difficult process of seeking treatment for substance use even more challenging. At the micro-level, stigma is linked with myriad adverse outcomes, including delayed treatment to avoid being labeled as a drug user, risky behaviors like needle sharing, and dishonesty about substance use with others, even healthcare providers.
Lack of Privacy
The overall lack of privacy can also be a barrier to treatment for those in rural communities when it comes to substance use. Even if someone acknowledges that they want to seek help, they may feel deterred simply because they’re afraid of being recognized while doing so. The stigmatization of substance use is a large contributor to these kinds of fears.
After all, what if a neighbor or community member saw them at a clinic or needle exchange program? The fact that someone was accessing services could then be spread to others in the community, resulting in further stigmatization, shame, and isolation. These feelings can be further exacerbated if a community member is a provider of these services.
Privacy concerns can be so powerful that people may avoid seeking treatment altogether. Even if they initially seek treatment, they may delay or forgo necessary follow-up care to maintain their anonymity. Ongoing support and care are vital to recovery and avoiding relapse in the future.
Cultural Norms
Cultural norms in rural areas can impact how people view and respond to opioid use. Though each place is unique, it’s common for rural communities to prioritize values in America. Inherently, rural areas have low population densities and are often far from cities, towns, and other population centers. It’s only natural that citizens of these areas tend to take care of themselves and each other rather than seek outside help.
Additionally, rural communities are more likely to distrust the healthcare system due to long-standing and ongoing issues when they do engage with it. Rural residents may not consider outside treatment as a viable option for themselves, even if they want to stop using substances.
Valuing self-reliance, coupled with stigma and privacy concerns, can result in rural communities steering clear of or discouraging discussions of addiction altogether. People may feel they have to manage their problems on their own to avoid their neighbors viewing them as a moral failure. This can cause individuals in rural areas to feel alone in coping with their substance use, as both external and internal support systems seem to be unavailable.
Access Gaps
In addition to social and cultural factors, significant logistical barriers affect rural residents’ ability to seek care. In particular, it’s challenging for people in these communities to actually access healthcare services due to physician shortages. Though these shortages impact all areas of the U.S., rural communities are particularly affected. Individuals living in rural areas may struggle to see a primary care provider, let alone access specialized opioid recovery services.
Additionally, people in rural areas may have to travel long distances to access healthcare at all. For instance, many have to travel almost twice as far as their urban counterparts to get to the nearest hospital. If they aren’t able to drive, actually traveling to healthcare services may be close to impossible, as there’s a low likelihood of reliable public transportation. That’s to say nothing of related challenges, such as time away from work or childcare, that can further complicate travel.
Healthcare access gaps can also worsen stigma and privacy concerns for rural residents. With fewer options available, people may be more likely to visit the closest healthcare facility to their community, which may be similarly convenient for their neighbors. For people seeking treatment for substance use, this increases the risk of being recognized as well as stigma after the fact.

Image Source: Pexels
Community-Centered Strategies for Reducing Stigma
The opioid crisis doesn’t just affect individuals; it impacts entire communities. To effectively reduce the stigma of addiction in rural areas, it’s vital to engage the community first and foremost.
Even well-intentioned top-down interventions are unlikely to resonate in areas that value self-sufficiency and independence or distrust major institutions. Ultimately, members of small communities may meet policies or mandates from a large governing body or programs from an outside health program with suspicion, rather than embracing them with open arms.
That’s why enlisting the help of local institutions and leaders is so critical. Community-based approaches have been linked to successfully improving knowledge of opioid use and treatment. People and groups that community members already trust are far more likely to have the desired impact in fighting stigma. They understand the unique needs, concerns, and dynamics of their communities and can use their voices to spread the message in ways that resonate with their neighbors.
Education-First Public Health Messaging
Reducing stigma begins with education about the realities of opioid use and treatment options. All messaging should be evidence-based, focusing on the facts of substance use disorders and avoiding the incorporation of morality or judgment.
Educational materials should frame substance use as a complex and chronic health condition rather than a personal failing. They should include fundamental information, including risk factors for opioid use and options for recovery and treatment. They should also go over the proper language to use when discussing substance use to avoid further stigmatization. This kind of information is key to challenging existing beliefs, dispelling misinformation, and encouraging people to seek and accept help when needed.
In rural areas, consider engaging with:
- Schools (with messaging tailored to be age-appropriate) and parent groups, such as parent-teacher associations
- Churches and religious groups
- Non-profits or advocacy groups, such as mental health organizations or homeless shelters, that work with or might support individuals impacted by substance use
- Local 12 Step programs, such as Alcoholics Anonymous or Narcotics Anonymous
- Clinics in the area that provide relevant services, like needle exchanges or methadone clinics
- Local businesses or agencies that do work related to mental health, substance use, or public health
These groups can act as messengers and help adjust educational materials to maximize impact for their specific audiences. Additionally, they may have ideas for other organizations to engage with or individuals who could help spread further awareness.
Normalizing Recovery Through Community Leadership
Local leaders play an essential role in shaping community attitudes about addiction in rural communities. If an individual is well-regarded and trusted by others, their words carry significant weight, giving them the power to help others question deeply held beliefs.
Many different kinds of people can serve as community leaders, from elected officials to business owners to dedicated parents. No matter who they are, they share the ability to visibly advocate against stigma and for recovery at the community level. They can work to garner public support for increased education about opioid use and treatment in their areas. That can take just as many forms, ranging from social media campaigns to speaking or volunteering at in-person events.
What’s more, local leaders can use the power of storytelling in their advocacy. They can use their own existing platforms to elevate others’ voices, including those who are in recovery from opioid use and working to improve substance use education. Not only does this help other people and groups earn trust from communities, but it can also cultivate a more profound sense of urgency and empathy in addressing the opioid crisis by showcasing its very real impacts on human life.
Protecting Privacy While Expanding Access to Care
There remains a tension between preserving patient privacy and expanding access to care in rural environments. This is why privacy needs to be at the forefront of strategies used in these communities. Privacy-preserving solutions, such as telehealth and out-of-community treatment options, are essential to effective, ongoing engagement with care.
Telehealth and Remote Treatment Options
Telehealth and other remote technologies can overcome some of the social and logistical barriers to receiving treatment for opioid use in rural areas. There are many different kinds of remote treatments available, such as:
- Initial screenings, diagnoses, and consultations
- Addiction counseling
- Individual and group therapies
- Medication-Assisted Treatment (MAT)
- Follow-up care
By using telehealth appointments at home, people can preserve their privacy while still accessing the care they need. It can help reduce the impact of stigma, as people can receive treatment without worrying about being recognized or publicly scrutinized, or how it will impact their standing in the community.
Additionally, telehealth makes it easier for individuals in rural areas to access care overall. They can undergo treatment from the comfort of home and don’t have to travel long distances to see healthcare providers. This can also reduce the need to take time off from work or to find childcare during appointments. Telehealth also improves continuity of care, allowing rural residents to see the same providers for follow-up care.
Regional and Out-of-Community Treatment Models
Regional and out-of-community treatment models may be another impactful option in addressing the rural opioid crisis. These treatment models allow patients to find care outside of their immediate communities, thereby improving overall access. They may also be a helpful alternative for people who distrust large, traditional healthcare institutions in the closest major city.
It’s essential to increase awareness of treatment options that are near, but not actually in, specific communities. Leaving a community, especially an insular one, can reduce fear of social exposure and make patients feel more comfortable taking the initial steps toward recovery. It can also make it easier to keep up with any necessary follow-up care.
These models have the greatest chance of success with coordinated support efforts, such as referral networks and practical assistance to access care. Local organizations, ranging from clinics to social service providers to health departments, can partner with regional providers to streamline the referral process. Similar support networks can help with transportation, such as shuttle services or gas vouchers. This, in particular, allows for discreet access to care while simultaneously addressing logistical hurdles.

Image Source: Pexels
Building Trust Between Rural Communities and Recovery Providers
Though options like telehealth and regional treatment networks are beneficial, distrust between rural residents and providers persists. Improving awareness and making treatments more available are great first steps, but it’s vital to build rural communities’ trust in those who are actually providing them with care.
Specialized local treatment centers for substance use can address some of these challenges in rural areas. Many have discreet intake processes designed to reduce patient stress, allowing individuals to focus on getting the treatment they need. Additionally, recovery providers may offer hybrid care models, allowing patients the flexibility for privacy-protecting remote care if that works better for their needs.
Treatment centers can also complement local support systems and participate in regional networks. That could take many forms, such as providing transportation to appointments, putting on a local winter coat drive, or collecting food donations for residents in need. These kinds of services allow providers to integrate into local support networks and demonstrate that they’re a reliable part of and care about the community as a whole — not an outside establishment.
Supporting Long-Term Recovery in Rural Settings
Even with significant efforts, recovery from opioid use disorder is more than just getting initial treatment. It’s an ongoing process that takes time and may not be linear. Each recovery journey is as unique as the person embarking on it.
Simply put, there’s a need for sustained and accessible support structures. That’s why it’s as important to invest in supporting long-term recovery in rural settings.
Economic Stability, Employment, and Reintegration
Part of sustained recovery is helping individuals establish financial stability after initial treatment. Improved financial health is linked to better recovery outcomes, with difficulties in recovery more likely to arise from financial instability. Consistent, full-time employment is a significant part of achieving improved finances and recovery for many.
However, people who have used opioids face significant barriers to employment and considerable stigma in the workplace. Employers themselves play an essential role in reducing workplace stigma at various levels, and should make an effort to do so. Still, individuals may face other hurdles, such as transportation, legal troubles, or ongoing health issues, that make finding and holding full-time employment difficult.
That’s why employment support services are so valuable. Job training opportunities for people who are in recovery from opioid use can help them learn new, valuable skills, as well as establish healthy habits to maintain long-term employment. It’s equally important for employers to educate themselves on how to best support candidates and employees. Reintegration support from treatment providers or local organizations can also be helpful to individuals as they work to navigate any challenges that arise.
Ultimately, the opioid crisis has unique impacts in rural areas and requires strategies tailored to address those communities and their specific needs. Due to differences in cultural norms and the realities of daily life, what works well in an urban area is unlikely to work in a rural one, and what works for one rural area may not work for another. It takes dedicated, customized, and ongoing efforts to effectively address the rural opioid crisis and support residents on their road to recovery.
Resources for Rural Communities Facing an Opioid Crisis
Consider reviewing the resources below for additional information on supporting rural communities and their residents in the midst of an opioid crisis.
Crisis and Immediate Support Services
- 988 Suicide & Crisis Lifeline: Available 24/7 for individuals experiencing emotional distress, substance-related crises, or thoughts of self-harm. Support is available via call, text, or chat and can be accessed regardless of geographic location.
- Crisis Text Line: Provides immediate, text-based crisis support for individuals feeling overwhelmed, isolated, or in emotional distress. This option can be invaluable for those seeking discreet support in rural settings.
- Poison Control (1-800-222-1222): Offers immediate guidance in cases of suspected overdose or medication-related emergencies, including opioid exposure.
- Freeman Recovery Center Emergency Admissions: Offers immediate same-day admissions for people seeking treatment for substance use addictions.
Federal and National Substance Use and Recovery Resources
- SAMHSA National Helpline (1-800-662-HELP): A free, confidential, 24/7 helpline offering treatment referrals and information for individuals and families facing substance use disorders.
- National Institute on Drug Abuse (NIDA): Offers research-based information on opioid use disorder, evidence-based treatment approaches, and prevention strategies.
- Health Resources and Services Administration (HRSA): Supports access to healthcare in rural and underserved communities through federally qualified health centers, rural health clinics, and funding initiatives aimed at expanding substance use treatment and behavioral health services.
Rural-Specific Health and Recovery Support Organizations
- Rural Health Information Hub (RHIhub): A national clearinghouse for rural health data, toolkits, funding opportunities, and evidence-based program models. RHIhub offers extensive resources on rural opioid use disorder treatment, recovery support, and community-level interventions.
- National Rural Health Association (NRHA): Advocates for improved healthcare access in rural communities and provides educational resources related to behavioral health, substance use treatment, and workforce development in rural settings.
Nonprofit and Peer-Led Recovery Organizations
- National Alliance for Recovery Residences (NARR): Supports evidence-based recovery housing standards and maintains directories of certified recovery residences, including options serving rural populations.
- Faces & Voices of Recovery: A national advocacy organization focused on recovery community engagement, public education, and stigma reduction. Offers resources that elevate lived experience and peer leadership.
- SMART Recovery: Provides science-based mutual support groups for individuals recovering from substance use disorders, with both in-person and online meeting options to accommodate rural participants.